Dr. John Ngendo (left, inside the high-risk zone) refers to a patient chart with our Medical Activity Manager, Dr. Jean-Patrick Ouamba

Ping among the patient wards inside the high-risk zone at the MSF Ebola Treatment Centre in Bunia, DRC.
Ka-Ping Yee is a software engineer who recently returned from working at an Ebola Treatment Center during the epidemic in the Democratic Republic of the Congo. He helped develop tools for Doctors Without Borders, an international network founded in 1971 that sends help to medical crises around the world. After Ping came home to Berkeley in early 2020, I got him on the phone to learn about what it means to innovate on an Ebola field mission.
Editor’s Note: Doctors Without Borders originated in France. In French, their name is Médecins Sans Frontières, so it’s abbreviated as MSF rather than DWB. Also: Most virus names are not capitalized; however, the name of the Ebola virus is capitalized because it’s named after the Ebola River, where the first outbreak appeared.
LYDIA LAURENSON: How did you end up working with MSF? What did you build for them?
KA-PING YEE: I grew up and got my engineering degree in Canada. After attending grad school at UC Berkeley, I became interested in humanitarian and world affairs, and went to work for Google.org [Google’s charitable arm]. In 2010, I helped start the disaster response team, Google Crisis Response, and stayed there until 2015. When I left Google, I started working freelance in the same space, and I’ve been privileged to do several projects with MSF.
[[This article appears in Issue One of The New Modality. Buy your copy or subscribe here.]]
For the Ebola mission, I helped build an EMR, an electronic medical record system that can be used on a tablet (like an iPad). This is useful because paper doesn't work very well in an Ebola setting, even though that's still the standard practice. For one thing, paper isn’t very durable. Conditions can be very humid or wet in field clinics, so it might fall apart. Also, medical staff wear protective equipment, like gloves and goggles. That hinders their writing and makes it hard to read. Most importantly, the patients are kept in isolation, and there are strict rules about how you interact with the “High-Risk Zone.” Objects are generally not carried out of the High-Risk Zone. You can carry things in, but you cannot take things out.
So conveying information you've written on a piece of paper is a big hassle. Either you read it aloud and someone outside copies it down, or you hold it out for them to read. I once saw a photo of someone dressed in protective equipment, with the goggles and everything, leaning over a fence and holding out a piece of paper. A person on the other side of the fence was taking a photo of it with their cell phone.
That's been the state of the art — people taking pictures of handwritten scrawls, and then later opening up the photo on the cell phone after taking off all their equipment. They’d sit down in the office, squinting at these grainy photos on their phones, trying to re-transcribe their notes. So we built an EMR to solve these problems.
LYDIA: One thing that strikes me about your solution is how low-tech it is. The complicated part is not the tech, it’s understanding the need behind it.
PING: For many attempts to bring technology into the developing world, it's difficult to aim at the right set of user needs. You have to really understand the situation, the context. In this case, a huge amount of effort went into making the software interface understandable for people without much training. To do that, we conducted many, many interviews with doctors and nurses who'd just returned from the field. We did role-plays. We even had them dress up in real protective gear and test the tablets while we splashed them with chlorine solution.
We also chose to use inexpensive parts, components that field workers could buy locally. For example, everything — the server, the wifi network, the tablets — is powered from a 12-volt battery. Someone in the Congo could charge up a car battery, or a motorcycle battery, and run our system off that.
LYDIA: So a lot of what you took away from your work wasn’t about technical innovation.
PING: No. But I learned a lot about public health innovation. One thing that confused me before I arrived in the Congo was reports of armed groups attacking Ebola Treatment Centers. In February 2019, an ETC was shot up and burned to the ground. It was shocking. I couldn't understand it — why would anyone attack the people trying to save them from a deadly epidemic?
It became clear once I spent some time there. Previously, I was only seeing a tiny part of the picture.
For us in the USA, Ebola is extremely scary. And it’s very lethal, but it’s far from the largest problem in the DRC. When I was there, the country had about 4,000 Ebola cases — but over 200,000 measles cases. This measles epidemic has killed more people than the Ebola epidemic. The Congo has measles epidemics all the time, and we never hear about them. But Ebola draws international attention. It’s a big business, as ugly as that sounds.
So imagine being a villager in the Congo. You see kids in your community dying of measles every year, and no one shows up to help you. Then Ebola happens, and suddenly there are NGO trucks everywhere, and rich foreigners appear in your country, all earning unthinkable salaries by your standards.
LYDIA: And the reason for that international response is that First World nations are afraid of Ebola, but we're not afraid of measles?
PING: Right. We've forgotten that measles exists. Measles might have a bit of a comeback with the anti-vaccination movement, but generally, the First World has it handled. So it's not a sexy disease to report on. But measles is incredibly contagious.
Ebola, on the other hand — it’s not that contagious, but it has a fatality rate of 60% to 80%. There are scary movies about it, and there’s still no cure anywhere. We had a single Ebola case arrive in the United States in 2015, and the entire country freaked out. That kind of attention distorts our picture of what's going on over there. They face so many more problems, day in and day out, year after year.
LYDIA: To them, it looks really cynical on our part. We help with the one problem we share with them, and none of the problems that we don’t share.
PING: Not only that, but people make a lot of money from the international response. For every Ebola epidemic, an entire sub-economy springs into existence. When outside nations pour hundreds of millions of dollars into an economy like the Congo, it distorts everyone’s incentives. The magnitude of the strangeness isn't clear to us from the outside.
One reason I’m so grateful to work with MSF is that they choose to act in ways that highlight long-term structural issues, not just medical issues. In many domains, they’re the best responders in the world, certainly to Ebola, but many other things as well. Because they have this extraordinary competence and reputation, they can be independent of any political actor, and they can use their voice to speak out about what they see. A key concept in the MSF ethos is témoignage, the French word for “witnessing.”
There are crises everywhere. There are parts of the world where you could just throw a dart at a map and there’d be a crisis happening anywhere it hits. So from MSF’s perspective, the question becomes: How do you decide where to go? MSF knows they cannot replace national health systems. So in order to have a lasting impact, they choose places where they can both save lives and draw attention to injustice.
For example, MSF was active in rescuing refugees in the Mediterranean; they helped call attention to that crisis. Their actions with Ebola are similar. They call attention to human rights violations and show that there’s a better way, by treating Ebola patients first and foremost as people, not purely as disease vectors to be stamped out.
Let’s imagine you’re a health authority in an Ebola epidemic, and you learn there's a village where someone appears to have Ebola symptoms. You want to isolate that person so they won’t transmit the disease. Now think about trying to do this in a society torn by violence, with lots of areas controlled by armed groups.
If all you care about is isolating suspected cases as quickly as possible, you're focused on finding that person and getting them out of their village, to the nearest Ebola facility. You're probably going to travel with an armed escort to get through the dangerous parts of the country. And if you can't make people understand why you're taking someone away, you may use the threat of force to do it.
But there are only a few Ebola facilities in the country. So this means sick people get taken to places far away from home, where their families can't visit them, and they die alone. What their community experiences is friends and family members getting taken away, and coming back in body bags.
After you do that a few times, your reputation will make it impossible to operate. No one will trust you. Then people will do things like burn down your clinics, rather than allowing you to kidnap their sick family members.
In contrast, MSF has been operating for years in that part of the Congo, as a purely benevolent actor. Even when MSF went to villages with Ebola cases, they asked people what they needed, and they listened. Some of those people said they weren't interested in Ebola treatment — they needed maternity care or immunizations, so MSF did those things. Then when the people eventually decided they needed an Ebola isolation facility within the village, so patients could be visited by their families, MSF was ready to act. Even then, they offered choices. First, MSF explained, “Here are the requirements we have to meet to make the facility safe. These are some of the procedures we need to put in place to prevent transmission,” and then asked, "Within those constraints, how do you want it to look? What building materials would you like us to use? What color should it be?"
“It’s not just their medical skills. By paying attention to human rights, MSF achieves more than many other organizations.”
It’s not just their medical skills. By paying attention to human rights, MSF achieves more than many other organizations. With Ebola, they work to show that you don't have to use force — in fact, using force might be counterproductive. They use their competence to embarrass others into doing a better job.
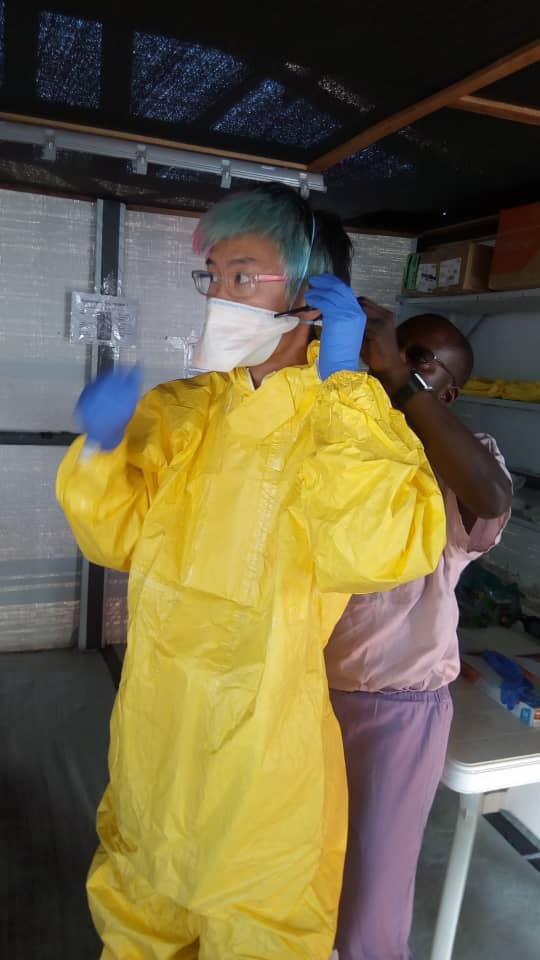
Ping dons Personal Protective Equipment in preparation for entering the high-risk zone at the MSF Ebola Treatment Centre in Bunia, DRC.
LYDIA: Thank you for sharing all this. Last question: You came home from the Ebola epidemic to the coronavirus pandemic. Do you have any advice?
PING: Well, my experience doesn’t necessarily give me expertise in this situation. This is a different context, and the resources available are completely different. But it did give me the sense that biosafety is about having protocols simple enough to be followed by everyone, consistently, until they become habits. One example of a protocol is that, in any Ebola context, MSF enforces a “No-Touch Policy” for all staff in the field. Not only do you not touch patients or medical staff — you don’t touch anybody, even your colleagues who might not be working in health facilities.
So you go for many weeks without handshakes, without hugs. I can say, on a personal level, this was really hard at first — but I did get used to it. It turned out to be easier than I expected.
It's surreal to see something like that playing out here. It’s hard right now, the social distancing. I certainly find it challenging. But I think it will eventually become a part of the rhythm of life.
[[This article appears in Issue One of The New Modality. Buy your copy or subscribe here.]]
Transparency Notes
This piece was written by Lydia Laurenson, editor in chief of The New Modality. NewMo did a light fact-check on some items (such as témoignage and the destruction of the clinic), but did not fact-check most things (such as Ping's engineering discussion). For more about our transparency process, check out our page about truth and transparency at The New Modality.


